REVISION KNEE REPLACEMENT
While modern total knee replacements are highly successful operations with many studies showing more than 90% survival at 15 years, a proportion of them will fail due to various reasons. This may require further revision surgery which is often a more complex than a primary total knee replacement (first time knee replacement).
The number of knee replacements done worldwide is increasing and catching up with the number of hip replacements being done. It is also being offered to relatively younger patients in whom knee replacement would not have been considered in the past. Inevitably the need for revision knee replacements is also increasing. While this has considerable impact on the resources of a health system, majority of the patients would have functional improvement following the revision procedure.
The surgeon has to deal with various technical problems including soft tissue problems, bone loss, infection etc., The surgery also requires special equipments and implants. While it would be possible to do revision surgery in majority of the patients, the medical co-
There are a number causes for failure of a knee replacement which may require revision surgery including:
With time, the plastic component of the knee replacement becomes worn out. In that process tiny plastic particles are produced to which the surrounding tissues react. This reaction leads to the bone getting gradually eaten away (lysis) leading to loosening of the knee replacement. The knee becomes painful and can become swollen due to the inflammation. Sometimes the loosening may be relatively asymptomatic for a long time and becomes only very symptomatic when there is large amount of bone destruction which makes the revision procedure even more complex. This is one of the reasons for regularly following the knee replacement patients with x-


Asepic Loosening
Infection following knee replacement is a very rare complication. It can occur soon after surgery (early infection) or many years after the hip replacement (late infection). Early infection can be superficial or deep. While the former may respond to antibiotics, the deep infection will need further surgery in the form of washout or revision procedure. Late infection can occur at anytime throughout the lifetime due to bacteria (bugs) entering the blood stream from infection in other parts of the body. If this happens, the knee replacement gradually becomes loose and the knee becomes painful and swollen. Although it is a challenging problem, majority of the patients could be treated by revision surgery. This usually is a two stage procedure with the first stage being removal of the infected knee replacement and insertion of temporary spacer and treatment with antibiotics. This is followed by second stage with a definitive revision knee replacement (when the infection has settled – usually after 3 months).

X-


After two stage revision surgery


Function six weeks after two stage revision
The bone fractures near the knee replacement. It is a rare problem and usually happens at the lower end of the thigh bone. Depending on the nature of the fracture, this could be treated by internal fixation or by revision of the knee replacement depending on the bone stock and whether there is loosening of the implant.
If the soft tissue balancing is not adequate, the knee may feel functionally unstable. This can also lead to early failure. If appropriate revision surgery could be contemplated with a more complex knee replacement which compensates the ligament imbalance.

X-

After revision with a hinge knee replacement
In this type of problem, the knee cap does not track properly and may become tilted or dislocated while bending the knee. This may be painful and may require revision surgery to correct the mal-
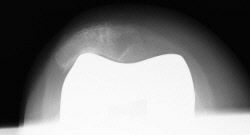
Skyline x-

The knee cap tracking normally after revision knee replacement with correction of malrotation of the components
Occasionally, the extensor mechanism may fail. This is a rare complication and may occur at the time of surgery with difficult knee replacements and revision surgery. It can also occur following an injury (tendon rupture or patella fracture). It is a difficult problem to treat and would depend on the nature of the injury as well whether the failure was acute (for example at the time of surgery) or chronic (late rupture). Options include direct repair, reinforcement with tendon grafts and in extreme cases, an extensor mechanism allograft. Very rarely, the knee may have to be fused which is again a challenging surgery in the revision knee replacement setting with bone loss.
Occasionally the knee replacement becomes stiff with less than adequate range of movement. Often it improves with intensive course of physiotherapy although it may require manipulation under an anaesthetic. Very rarely it may need revision surgery, but the outcomes are variable.
Extremely stiff knee with loose total knee replacement (done many years ago).

Preoperative x-
After revision surgery with extensive quadriceps release. Has much better flexion. Still has extensor lag. But is improving. Postoperative X-

(The following example is of a patient who had instability of the knee replacement, tibial malrotation and maltracking of the knee cap)

Preoperative AP x-

Valgus stress showing instability

Skyline view showing knee cap is maltracking (out of place)

Superimposed CT scan picture showing internally rotated tibial tray
Preoperative valgus instability
Preoperative function –

She underwent revision knee replacement with a hinge knee prosthesis and correction of tibial rotation. X-
Comparison of preoperative and postoperative function showing considerable improvement in the immediate postoperative function –

Preoperative skyline view

Postoperative skyline view
Comparison of preoperative and postoperative function showing considerable improvement in the immediate postoperative function –
Preoperative function
Postoperative function
Comparison of preoperative and postoperative stability to valgus stress
Preoperative valgus instability
Postoperative stability
The following are some relevant selected scientific references:
1. Younger age increases the risk of early prosthesis failure following primary total knee replacement for osteoarthritis. A follow-
Acta Orthop. 2010 Aug;81(4):413-
Julin J, Jämsen E, Puolakka T, Konttinen YT, Moilanen T.
Medical School, University of Tampere, Finland.
Abstract: BACKGROUND AND PURPOSE: Total knee replacements (TKRs) are being increasingly performed in patients aged < or = 65 years who often have high physical demands. We investigated the relation between age of the patient and prosthesis survival following primary TKR using nationwide data collected from the Finnish Arthroplasty Register.
MATERIALS: From Jan 1, 1997 through Dec 31, 2003, 32,019 TKRs for primary or secondary osteoarthritis were reported to the Finnish Arthroplasty Register. The TKRs were followed until the end of 2004. During the follow-
RESULTS: Crude overall implant survival improved with increasing age between the ages of 40 and 80. The 5-
INTERPRETATION: Young age impairs the prognosis of TKR and is associated with increased revision rates for non-
2. The epidemiology of revision total knee arthroplasty in the United States.
Clin Orthop Relat Res. 2010 Jan;468(1):45-
Bozic KJ, Kurtz SM, Lau E, Ong K, Chiu V, Vail TP, Rubash HE, Berry DJ.
Department of Orthopaedic Surgery and Philip R. Lee Institute for Health Policy Studies, University of California, San Francisco, 500 Parnassus Ave., MU320W, San Francisco, CA 94143-
Abstract: Understanding the cause of failure and type of revision total knee arthroplasty (TKA) procedures performed in the United States is essential in guiding research, implant design, and clinical decision making in TKA. We assessed the causes of failure and specific types of revision TKA procedures performed in the United States using newly implemented ICD-
3. The increasing financial burden of knee revision surgery in the United States.
Clin Orthop Relat Res. 2006 May;446:221-
Lavernia C, Lee DJ, Hernandez VH.
Orthopaedic Institute at Mercy Hospital, Miami, FL 33133, USA.
Abstract: The popularity of total knee arthroplasty combined with the aging US population indicates a dramatic increase in revision TKA procedures. Our objective was to project revision surgery costs in the United States, and to estimate the financial burden for hospitals historically under-
4. Cost effectiveness of revision total knee arthroplasty.
Clin Orthop Relat Res. 2006 May;446:29-
Burns AW, Bourne RB, Chesworth BM, MacDonald SJ, Rorabeck CH.
London Health Sciences Centre, University of Western Ontario, London, Ontario, Canada.
Abstract: Total knee arthroplasty now exceeds total hip arthroplasty as the most commonly performed joint replacement. Projections suggest the need for revision knee arthroplasty in the future will produce an immense economic burden. The excellent cost effectiveness of primary knee arthroplasty has been well established. This article explores the cost effectiveness of revision knee arthroplasty, and makes a comparison of costs between different international health care systems. While revision knee arthroplasty is more costly, technically difficult, and complicated than primary knee arthroplasty, it is still a cost effective means of improving function, pain relief, and quality of life. The role of national arthroplasty registries will be important in guiding decision making toward reducing the requirements for revision surgery.
5. Prevalence of primary and revision total hip and knee arthroplasty in the United States from 1990 through 2002.
J Bone Joint Surg Am. 2005 Jul;87(7):1487-
Kurtz S, Mowat F, Ong K, Chan N, Lau E, Halpern M.
Exponent Inc., 3401 Market Street, Suite 300, Philadelphia, PA 19104, USA.
Abstract: BACKGROUND: The purpose of this study was to quantify the procedural rate and revision burden of total hip and knee arthroplasty in the United States and to determine if the age or gender-
METHODS: The National Hospital Discharge Survey (NHDS) for 1990 through 2002 was used in conjunction with United States Census data to quantify the rates of primary and revision arthroplasty as a function of age and gender within the United States with use of methodology published by the American Academy of Orthopaedic Surgeons. Poisson regression analysis was used to evaluate the procedural rate and to determine year-
RESULTS: Both the number and the rate of total hip and knee arthroplasties (particularly knee arthroplasties) increased steadily between 1990 and 2002. Over the thirteen years, the rate of primary total hip arthroplasties per 100,000 persons increased by approximately 50%, whereas the corresponding rate of primary total knee arthroplasties almost tripled. The rate of revision total hip arthroplasties increased by 3.7 procedures per 100,000 persons per decade, and that of revision total knee arthroplasties, by 5.4 procedures per 100,000 persons per decade. However, the mean revision burden of 17.5% for total hip arthroplasty was more than twice that for total knee arthroplasty (8.2%), and this did not change substantially over time.
CONCLUSIONS: The number and prevalence of primary hip and knee replacements increased substantially in the United States between 1990 and 2002, but the trend was considerably more pronounced for primary total knee arthroplasty. CLINICAL RELEVANCE: The reported prevalence trends have important ramifications with regard to the number of joint replacements expected to be performed by orthopaedic surgeons in the future. Because the revision burden has been relatively constant over time, we can expect that a greater number of primary replacements will result in a greater number of revisions unless some limiting mechanism can be successfully implemented to reduce the future revision burden.
